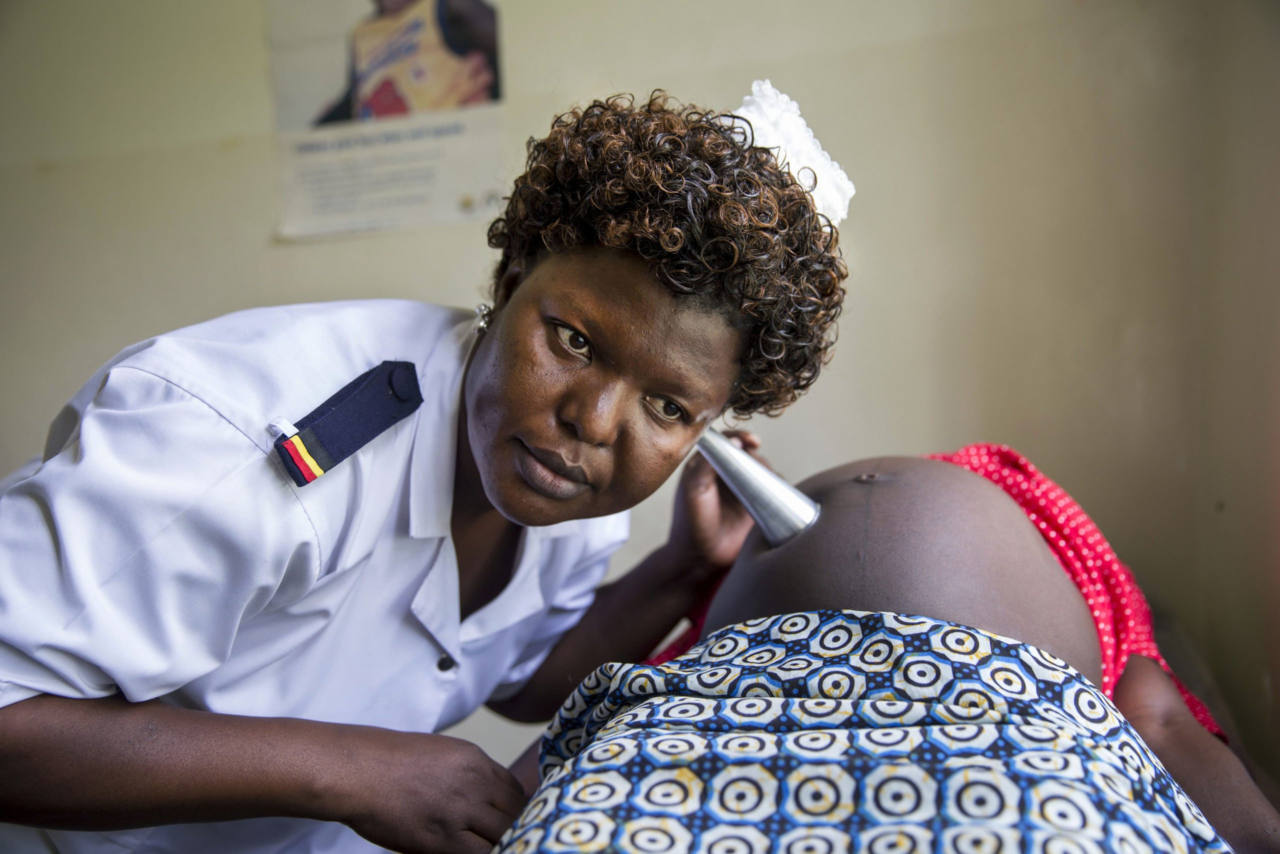
Although most women receive prenatal care during their pregnancy – providing an outstanding opportunity to reach them – many are never screened for syphilis.
Each year, one million pregnant women have active syphilis infections across the world – and a majority go untreated, resulting in over 350,000 severe adverse outcomes. This includes 143,000 stillbirths, 61,000 neonatal deaths, 41,000 preterm births, and 109,000 children born with severe disability due to congenital syphilis, which occurs when a mother with syphilis passes the infection on to her baby during pregnancy.
An inexpensive (less than US$0.50) shot of penicillin prevents the vast majority of the adverse outcomes, yet less than 30% of infected women are treated in many high-burden countries. The primary challenge lies in diagnosing syphilis in the first place. Although most women receive prenatal care during their pregnancy – providing an outstanding opportunity to reach them – many are never screened for syphilis.
A Simple Solution
Introducing HIV/syphilis dual tests, which cost just ~$0.15 more than HIV-only tests, would immediately increase syphilis testing such that it’s on par with existing HIV screening, and would thereby ensure millions more women are screened for syphilis every year.
Dual HIV/syphilis rapid tests offer an opportunity to dramatically and sustainably increase syphilis screening and treatment by leveraging the decades-long investment in health infrastructure related to HIV screening in pregnancy. Introducing HIV/syphilis dual tests, which cost just ~US$0.15 more than HIV-only tests, would immediately increase syphilis testing such that it’s on par with existing HIV screening, and would thereby ensure millions more women are screened for syphilis every year.
In 2020, Evidence Action launched our five-year maternal syphilis screening and treatment program in Liberia and we are well on our way to achieving our targets in the country. Through our partnership with Liberia’s National AIDS and STI Control Program, we have so far trained healthcare providers on the dual HIV/syphilis test in five out of fifteen counties, reaching 67% of pregnant women nationally. As a result, syphilis screening has risen from 6% to 39% nationally and Liberia has gone from having only six healthcare facilities providing HIV/syphilis dual screening and syphilis treatment to 269 facilities providing these services in less than two years. By the end of the five-year program, we aim to see at least 150,000 more pregnant women tested for syphilis every year and prevent more than 10,000 adverse birth outcomes over the five years.
Expanding Our Impact
Following the rapid success of the program model in Liberia, we looked to additional geographies where the program could be highly cost-effective and impactful. In considering program expansion, Evidence Action evaluates several criteria including: syphilis prevalence and incidence, high utilization of prenatal care, an existing gap between HIV and syphilis screening rates, political will supporting adoption of HIV/syphilis dual testing, and perceived interest in a partnership with Evidence Action.
After conducting a rigorous assessment, we ultimately sought expansion into Zambia and Cameroon; both of which have substantial disease burden. Zambia has ~800,000 pregnancies annually and a syphilis prevalence of 3.0%, and Cameroon has ~1 million pregnancies annually and a syphilis prevalence of 5.63%.
In late 2022, Evidence Action received a ~US$15 million grant from GiveWell to pursue a five-year maternal syphilis program in Zambia and a six-year program in Cameroon. While Zambia’s policies already advocate for dual testing, Cameroon is on the precipice of adopting a similar policy. An additional year for the Cameroon program allows our in-country leadership to support the government’s policy adoption, which is often a lengthy process. While our program model aims to provide governments with comprehensive support to successfully scale up HIV/syphilis dual testing, what this looks like in practice varies from country to country. For example, syphilis treatment in Liberia is provided at no-cost, whereas Cameroon has a fee-based healthcare system and pregnant women are expected to pay for treatment. As a result, we will be working closely with the Cameroonian Ministry of Health to identify national strategies to reduce or eliminate fee-based treatment for pregnant women; this is particularly timely given that the country is defining guidelines for a universal health coverage benefits package for pregnant women and children in the coming months.
In Zambia, there are at least 24,000 instances where syphilis is very likely to pass from mother to child and leave the unborn child vulnerable to stillbirth, neonatal death, and the complications of having either congenital syphilis and/or low birth weight. In fact, the incidence of neonatal deaths continues to rise in Zambia while other adverse health indicators have fallen. Zambia has both high prenatal care attendance and HIV screening rates, at 95% and 93% respectively. Through our partnership with the Ministry of Health’s National Prevention of Mother-to-Child Transmission and Laboratory Teams, we aim to scale dual HIV/syphilis testing to all 10 provinces across Zambia with the ultimate goal of closing the gap between HIV and syphilis testing.
In Cameroon, we will similarly seek to leverage the existing prenatal care HIV testing infrastructure across the country to introduce the dual HIV/syphilis test to all 10 regions in Cameroon. With almost 1,000,000 pregnancies a year, once the program reaches all facilities across the country, an additional 300,000 women will be screened for syphilis each year. The first year of the program in Cameroon will require planning and coordination with the various Ministry of Health departments, with a primary aim of including dual testing as a part of national policy. By working with the government to include the dual test in national prenatal care and HIV testing guidelines, the use of the dual test will be operationalized and solidified in policy and procedures for the long term.
As our expansion efforts launch in late 2022/early 2023, we look forward to our continued progress in Zambia, Cameroon, and Liberia to ultimately improve the lives of hundreds of thousands of pregnant mothers and their newborns. We don’t plan to stop there; in 2023, we will be looking to secure funding for a program in Nigeria, and exploring further expansion into other high burden countries to continue broadening our impact.