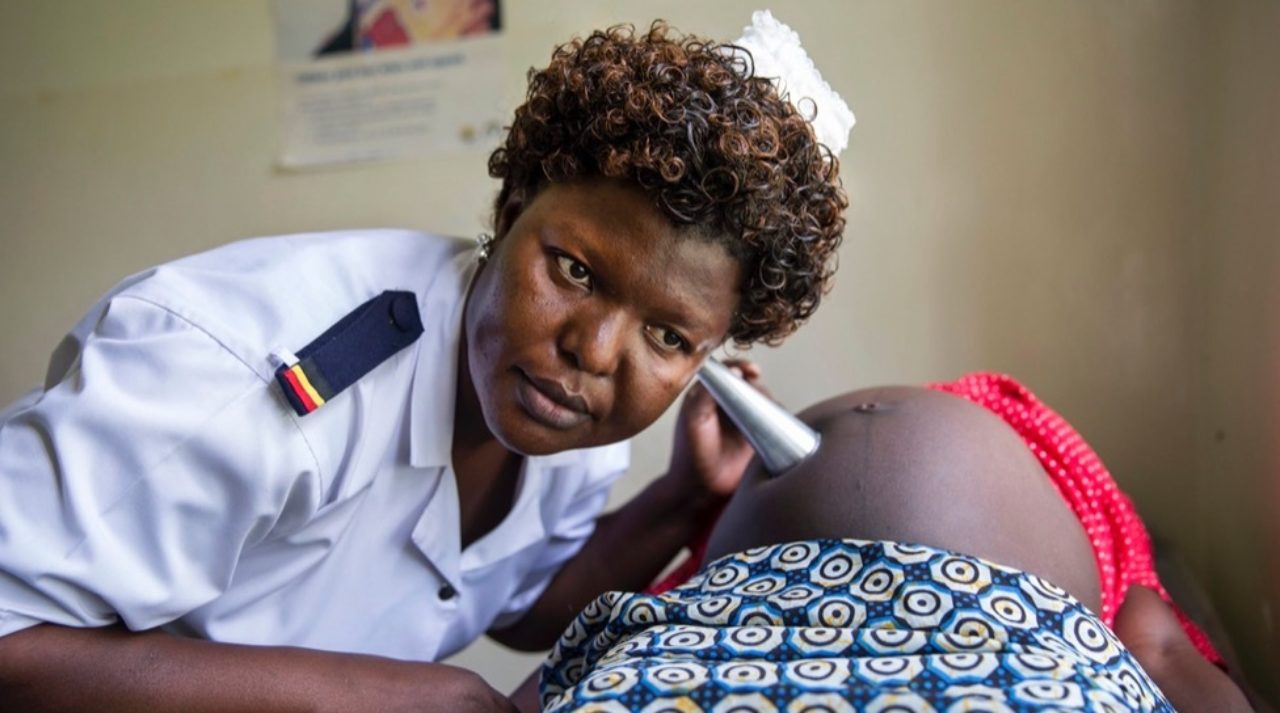
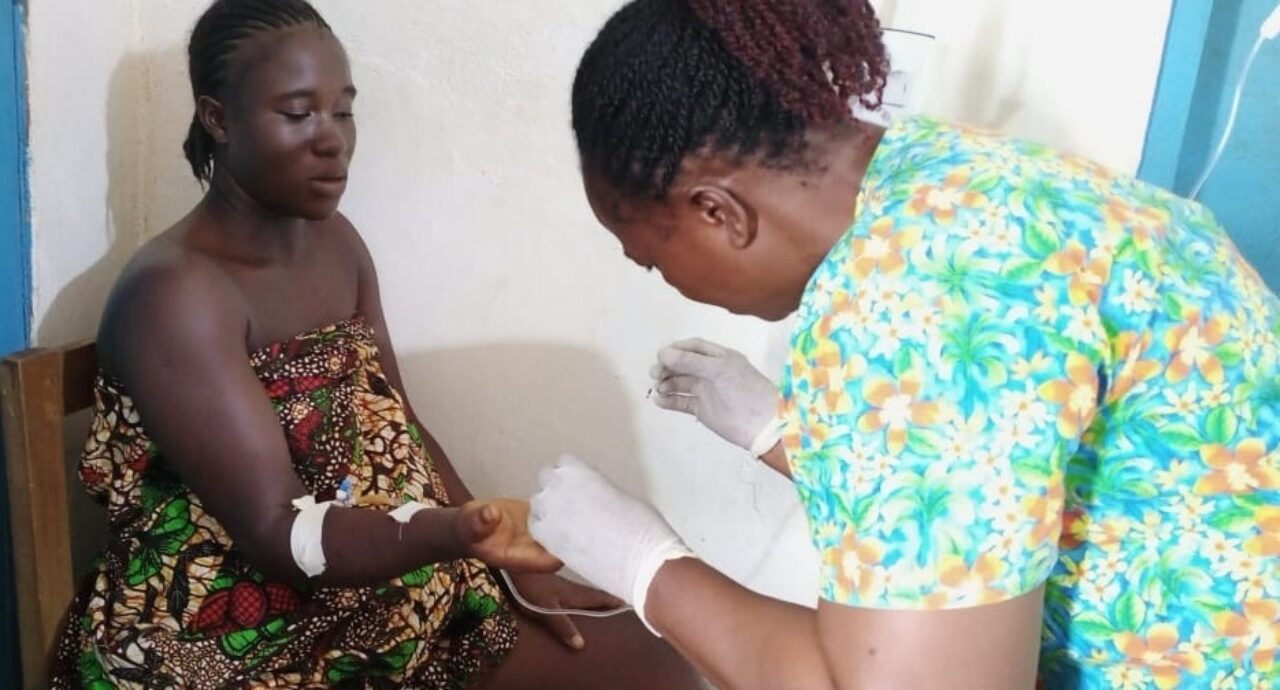
Everything we do is based on evidence and data. We focus on the most urgent needs and the biggest opportunities to combat global poverty. We only implement solutions that we know are proven to work. And we deliver outsized impact for every dollar.
Discover how we work