Update: Read our 2024 wrap-up: what we tackled, what we didn’t, and why for our progress on these goals.
What do micronutrient deficiencies, cervical cancer, untreated water, and parasitic worms have in common?
They’re all global health issues that you might not hear about too often, but they’re at the top of our priority list for 2024.
Part of our unique approach here at Evidence Action is addressing neglected global health challenges — those that have been ignored or underfunded for too long. We leverage rigorous research to find proven, cost-effective solutions — and then we put them into action, changing and saving millions of lives.
We had tremendous success throughout our first decade of outsized impact — scaling our life-changing interventions to over 500 million people globally – but there is still a great deal of work to be done. With the help of our supporters, we’re moving into the new year with highly ambitious goals and big plans for growth.
Here are six of the ways we’re going to tackle neglected global health challenges in 2024 – along with opportunities for you to support this critical work.
1. Making water safe to drink for millions in India through water treatment.
We’re taking on one of the biggest safe water projects in history — one that could ultimately bring lifesaving safe water access to 400 million people.
We’re working with the Government of India’s Jal Jeevan Mission, which has a mandate to bring safe water access to all rural households. We’ll be working closely with the Mission and two state governments as they continue to expand their reach, leveraging their infrastructure investment (household taps) as we help them install chlorination devices that will make household water safe to drink.
Our Safe Water Now program is meeting a specific, often overlooked need — few organizations are focused specifically on water treatment like we are. Most focus on building infrastructure, but the truth is, that’s simply not enough to save lives. Untreated water, even from an improved source, can be just as dangerous.
Water treatment is proven to be one of the most cost-effective ways to save children’s lives.
For a low additional cost, governments can deliver enormous health benefits by incorporating water treatment into the infrastructure that is enabling water access – and that’s exactly what we’re supporting the Government of India to do.

We’ve completed our pilot, which tested chlorination devices within the context of Indian water systems. With the government having accepted our recommendations from the pilot, we’re now preparing to launch technical assistance in two states in 2024. With our years of experience providing technical assistance in India, combined with our expertise in scaling water treatment across Africa, we are well-positioned for success. We’ll develop an optimized service delivery model and run it hand-in-hand with the state governments, while building their capacity to eventually take over.
Beyond the two initial states, our goal is long-term impact across the entire country. We’ll be working with the national government on the development of policies and guidelines that can be disseminated to other states, enabling nationwide scale with a goal of reaching hundreds of millions of people.
Give to the Safe Water Now Fund to support more opportunities like this.
2. Fighting cervical cancer in low-income countries by improving access to the HPV vaccine.
Cervical cancer is most often caused by human papillomavirus (HPV), a common sexually transmitted infection. Globally, cervical cancer is the fourth most common cancer for women, and it’s especially deadly for women in low- and middle-income countries, where 90% of its deaths occur.
That imbalance is caused by inequitable access to the HPV vaccine. With 99% effectiveness in preventing the two most common strains and significantly reducing the risk of cervical cancer, the HPV vaccine is easily available and highly encouraged for adolescents in high-income countries. In the U.S., for example, 76% of children aged 13-17 received at least one dose in 2022. But that’s unfortunately not the case everywhere.
We’re planning to leverage our school-based delivery model to cost-effectively reach adolescent girls with the lifesaving HPV vaccine.
Our school-based model was first developed for Deworm the World, and it’s now also leveraged in Equal Vitamin Access. Our success in both programs has proven that working through schools is one of the most cost-effective ways to reach children with critical health services. Through our technical assistance model supporting government partners, school-based delivery leverages existing government infrastructure and resources, rather than building a network from scratch, and reaches children where they already are.
Our HPV vaccine intervention is currently moving through the later stages of our Accelerator, which is our engine for new program development. Throughout 2023, we investigated where HPV vaccination could be feasibly launched and cost-effectively implemented at-scale. We identified Malawi and India as potential opportunities, and are now seeking funding to scale HPV vaccination in those countries.
Give to the High Impact School Health Fund to help expand school-based interventions.
3. Saving more newborn lives by helping pregnant women overcome micronutrient deficiencies.
Another intervention that’s in the later stages of our Accelerator is multiple micronutrient supplementation (MMS) for pregnant women. MMS is designed to help women meet their higher requirements for essential vitamins and minerals during pregnancy — it’s analogous to the prenatal vitamins that many women in high-income countries take.
Evidence shows that MMS can be an effective, low-cost solution to micronutrient deficiencies, which are common among pregnant women in low- and middle- income countries and can cause poor pregnancy and birth outcomes. If taken regularly during pregnancy, evidence shows that the supplements with at least four micronutrients reduce low birthweight by 21%, stillbirths by 9%, and small for gestational age (SGA) by 10%.
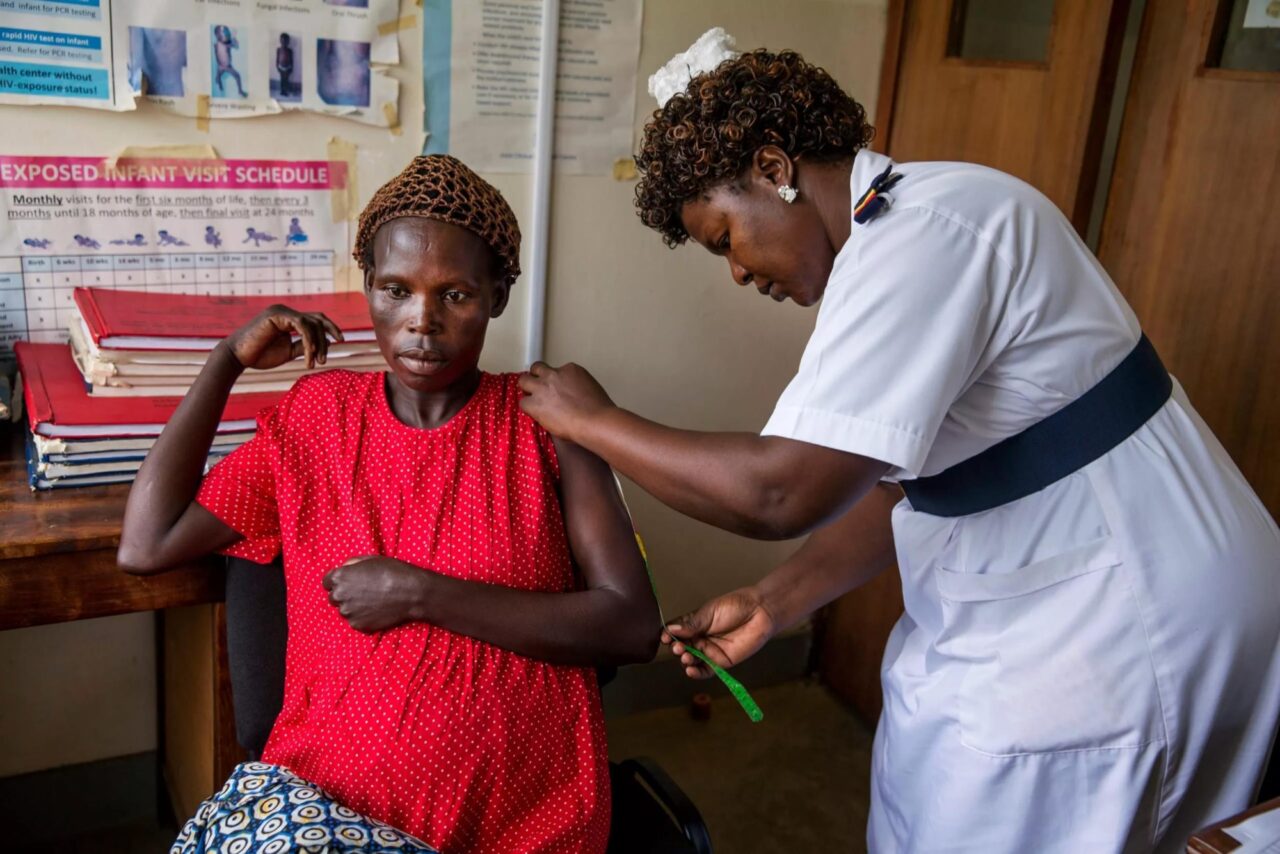
Despite its effectiveness, MMS has yet to be introduced in most countries at scale. To bring this life-saving and -improving intervention to women, we’re looking at the feasibility of scaling it cost-effectively through prenatal care systems — similar to what we’ve done with maternal syphilis testing and treatment. A big part of our testing is to understand what interventions are most effective in increasing adherence — because women need to regularly take MMS to reap the benefits.
We’ve been actively scoping this intervention in several countries across Africa and South Asia, and we’re planning to launch a two-year pilot in Nigeria to fully explore its impact potential for pregnant women and their newborns.
Give to the Radical Scale Fund to help us test other groundbreaking opportunities.
4. Helping millions of adolescent girls in Malawi beat anemia.
Our Equal Vitamin Access program is focused on reducing micronutrient deficiencies. Our first intervention in this program is iron and folic acid — weekly supplements that fight anemia.
Anemia can cause fatigue, weakness, and dizziness, but it also has severe impacts on physical and cognitive development for children and adolescents when left untreated — in fact, it’s a leading cause of disability in low- and middle-income countries.
Adolescent girls are especially susceptible to anemia once they begin menstruation — in Malawi, 45% of adolescent girls are anemic, compared to 32% of boys.
We started combating anemia in India in 2019, at the request of the government. Through our technical assistance partnership with the government, we leverage our Deworm the World model to also provide iron and folic acid supplementation, which is proven to reduce the risk of anemia by 49% among children aged 0-12 years. We’ve reached millions of children and adolescents in India, and now, we’re taking the fight to Malawi.
There are over 3 million anemic children in Malawi, and the disease is one of the top 10 causes of disability-adjusted life years (DALYs) among 5-19 year olds. Starting in 2024, we’ll be working closely with the Malawian government to scale the school-based delivery of iron and folic acid supplementation, alongside deworming (more on this below). We plan to cover all 29 districts in the country over the course of three years.
This means that millions of Malawian children — including adolescent girls — will feel stronger, be better able to stay in school, and have the chance to live up to their full potential.
Give to the High Impact School Health Fund to help us expand into Malawi and beyond.
5. Continuing to tackle underfunded neglected tropical diseases, and working ourselves out of a job.
Deworm the World has created extraordinary impact over the past decade. Our modeling indicates that the 1.8 billion treatments we’ve helped deliver to children (at just $0.50 per treatment on average) will likely generate $23 billion dollars in productivity gains by 2042.
And now, the program is at a turning point in some geographies — because the data shows that we’re winning the fight against worms.
Worm prevalence rates are dropping significantly in certain areas where we work. For example, a recent impact assessment in Kenya found that after nine rounds of consistent mass drug administration, the prevalence of soil-transmitted helminths — one of the diseases we treat – has plummeted from 32% in 2012 to just 6% in 2022. That's an incredible reduction of over 80%.
This is a very exciting indicator of success, and it means that mass deworming may soon no longer be needed there — and firstly in fewer areas of Kenya.

As we conduct impact assessments across our other geographies, we’ll be developing exit strategies for areas that now have worm infections under control. That means strategizing with our government partners on how we can responsibly shift treatment approaches — with the goal of possibly exiting entirely, and enabling governments to fully own the work going forward.
At the same time, we’ll be expanding the program into new places, like Malawi in early 2024, where funding shortfalls risk losing the gains made by the government and other partners in reducing the worm burden. We’re targeting delivery of 4.6 million deworming treatments across three years to continue to drive reductions in prevalence.
We’re proud to be part of a global movement that’s committed to combating neglected tropical diseases. That’s why we participated in the historic pledge at the 2023 Reaching the Last Mile Forum. And we remain focused on tackling the more underfunded NTDs, like soil-transmitted helminths.
Our deworming model is a low-cost solution that’s proven to work — and if we continue to invest in finishing the job we started, it’ll hopefully one day no longer be needed.
Give to the High Impact School Health Fund to help expand Deworm the World and other school-based programs.
6. Calling for safe drinking water to be on the global climate-health agenda.
We believe that there needs to be an increased focus on health solutions for the climate crisis — including for one of the most basic essentials for life: safe drinking water.
The health impacts of climate change have been shockingly neglected, although some recent progress has been made. For the first time, the COP28 climate summit in 2023 featured a Health Day, and the COP28 Declaration on Climate and Health calls for increased funding at the climate-health nexus.
But now we need greater funding commitments for proven health solutions that will protect people in the face of the escalating climate crisis.
Prioritizing safe water within climate resilience efforts cannot wait. Extreme weather events are exacerbating waterborne diseases like cholera, and increasing water scarcity means that access to safe water is poised to become even more out of reach for vulnerable communities.
The chlorination interventions that we use to treat water in Safe Water Now are proven to remove pathogens and make water safe to drink. We’re providing safe water access to over 10 million people across Africa today, and over the past decade estimate that this program has saved the lives of over 15,000 young children. As we continue to scale up Safe Water Now, we’ll be championing increased investment in climate-health solutions – especially for evidence-backed solutions like ours.
Give to the Safe Water Now Fund to help more communities build resiliency.



