Evidence Action’s Deworm the World Initiative calculates what it costs to deworm a child in the countries where we work. You might have seen the ‘cost per child per year’ to treat for parasitic worms cited in our materials and that of others.
So how do we calculate that cost? In the spirit of transparency (and in hopes of clearing up any misconceptions about how we determine our supported deworming programs’ cost per child), let’s talk costing!
Why Calculate the Cost of Deworming?
Miguel and Kremer’s 2004 seminal study analyzed the costs of school-based deworming and determined that it was less than $0.50 per child per year. At this low cost, deworming in schools is considered a ‘best buy for development’ given the long-term benefits that deworming provides to individuals and entire societies.
Of course, it’s now more than ten years later. Costs have evolved and programs have grown to reach millions more children in additional countries. So let’s take another look at this figure.
It’s important to note that understanding what a program costs does not measure its impact, and therefore our cost analysis is not used for a cost-benefit analysis. We don’t argue here that “with this amount of money we can cause a particular health benefit or educational outcome for a child.”
Rather, we simply say, “in this particular deworming program, here’s the total cost for each child treated” (the impact following from that treatment has been discussed at great length elsewhere). Because Evidence Action’s Deworm the World Initiative provides technical assistance and is one of a number of partners involved in a deworming program, we also consider costs incurred by other stakeholders such as implementing governments. We also track the costs of donated drugs when these are provided.
The school-based deworming programs we support are implemented by governments and vary greatly in scope. Thus, costs can be very different from state to state or country to country, as fixed costs are spread across a different number of children. Other variations also drive costs: the required drug(s) and frequency of their administration vary across countries depending on local worm infection prevalence and intensity. Some areas administer parasitic worm treatment alongside other health programs. This leverages existing infrastructure for deworming, potentially decreasing costs. In Delhi, the government has integrated treatment with its iron and folic acid supplementation program, requiring fewer resources dedicated to deworming alone. Another variation between countries is simply the cost of doing business — operating costs in Kenya, for example, are higher than those in India.
What Do We Include In Our Cost Analysis For Deworming And Why?
We follow J-PAL’s 2012 framework that offers guidance on costing large-scale programs in developing countries.
While we do include all partners’ expenditures in costing the deworming programs, we do not consider spending that would already be incurred without deworming taking place. Maintaining health departments and education systems creates costs that would exist even in the absence of deworming. We do not include these expenses in our analysis but focus instead on the additional costs resulting directly from implementing a deworming program.
Following a similar logic, we assume that teachers come to school on deworming day and the same amount of work gets done, in addition to the deworming activity. We thus do not calculate the value of alternative activities that teachers or government officials could be engaging in if not for the deworming program. Although this type of government contribution is not quantified in the model, we note that the existing platforms and infrastructure leveraged by school-based deworming is instrumental to the low-cost nature of these programs.
We also, as we noted, do not attempt to calculate the associated benefits of deworming to society in this analysis. So, what do we include in our calculation?
- Teachers’ and principals’ allowances: Our calculation includes per diems and travel allowances paid to teachers and principals when they attend deworming-specific trainings. Teachers’ and principals’ general salaries are not included because they do not spend additional time on deworming beyond what they are already compensated for by the government for regular classroom teaching.
- Drugs: We include the value of drugs in our calculation, whether the drugs are procured through donation from pharmaceutical companies via the WHO or purchased by the government.
- Prevalence surveys: We always include the cost of running prevalence surveys in our calculation because they are essential for informing treatment strategies and assessing the long-term impact of deworming. Surveys are done prior to deworming in a given geography to map worm prevalence and intensity and then, following rounds of deworming, subsequent surveys are conducted to understand the change in prevalence and intensity. Survey frequency varies across programs, but in general, survey costs are amortized across the treatment rounds they inform.
- Technical implementation assistance: Direct costs such as Evidence Action/Deworm the World staff time (both in-country and global) are included in our calculation because these costs are incurred in direct relation to program implementation. Indirect costs are also counted to cover functions like finance and HR that contribute to our support of the program.
- Community education and sensitization campaigns: We include all costs of designing and producing promotional materials in local languages. These are used to raise awareness about deworming and to encourage treatment participation and typically include TV or radio ads, village announcers, community parades, posters and fliers.
- Training: We include all costs of conducting trainings through a multi-tier cascade to equip government personnel from the national level down to the schools (and sometimes preschools) administering treatment. These include hiring qualified trainers, developing and printing materials, and lots of text messages and phone calls for coordination. When there are specific costs associated with training venues, we include them in the calculation. However, when training (as well as program-related meetings and other events) takes place in spaces that are government-owned and covered by their regular operational costs, those are not included.
- Monitoring and evaluation: We include all costs of data reporting, monitoring of deworming days and other critical events, and validating program coverage and results, including printing of forms, data entry and analysis, travel to school sites for activity monitoring, and outsourced or in-house data analysis.
TL;DR: Then What Is the Actual Deworming Cost Per Child Per Year?
Given all of this, what do we come up with when all is said and done? Here are our calculations for the most recently completed round of deworming in Kenya, and for the Indian states of Bihar, Rajasthan and Delhi where Evidence Action’s Deworm the World Initiative supports the national and state governments in their deworming programs.
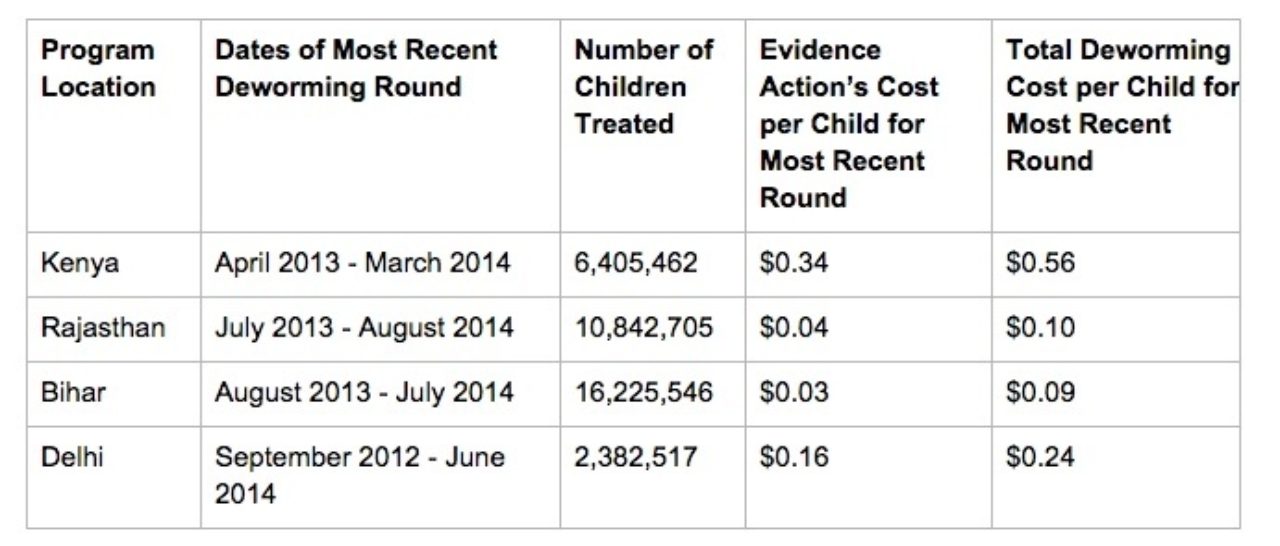
We include in this calculation the total fully loaded costs of deworming a child in each program location including expenditures from all partners — Evidence Action, government ministries, the World Health Organization, and others. We also break down our per-child costs for the program.
What explains some of these large discrepancies? Per-child treatment costs are higher in Kenya in large part because the national program is treating for schistosomiasis in addition to STH. This requires additional disease mapping and provision of the more expensive drugs to treat for schistosomiasis. Kenya also has different norms for allowances for government officials than India, and higher costs of doing business relative to India. Per-child costs are higher in Delhi than other Indian states, as there are relatively fewer kids treated. We are able to take advantage of economies of scale in Bihar and Rajasthan. No matter where in the world, however, school-based deworming remains a highly effective and low-cost program.