Don't gamble away NTD gains
After a decade of remarkable progress, neglected tropical diseases are on the retreat. But funding gaps threaten to undo hard-won victories. The evidence is clear: now is the time to invest big — or risk losing it all.
Support Deworm the World
The progress we've made on neglected tropical diseases is at risk.
Funding for neglected tropical diseases has collapsed. Official development assistance fell 41% between 2018 and 2023 — before USAID cuts made things worse. The World Health Organization's (WHO) 2025 Global NTD Report warns programs worldwide are being "severely disrupted," putting a decade of progress at risk.
The stakes are enormous. More than 627 million school-aged children remain at risk of parasitic worm infections. By interfering with nutrient uptake, these infections can lead to blood loss, malnourishment, and impaired development, posing a serious threat to children’s long-term health, education, and productivity. Without sustained funding, countries could see disease resurgence back to baseline levels.
But here's what makes this moment so critical: the programs are working. We know how to solve this problem. What we're losing is the resources to finish the job.
Evidence Action has proven what's possible.
Since 2014, Deworm the World has helped governments launch, scale, and sustain highly cost-effective school-based deworming programs. We’ve supported the delivery of over 2.2B deworming treatments to date, driving over $23B in productivity gains.
Recent impact assessments show significant prevalence reductions, enabling changes in treatment strategy and dramatically reducing the number of children needing treatment.
Kenya
A 2021-22 survey by Evidence Action and the Kenya Medical Research Institute shows several counties and sub-counties achieved the WHO's target for elimination as a public health problem. Prevalence of soil-transmitted worms has reduced by 82% since 2012, with 10 out of 27 counties reaching <2% prevalence, the threshold at which mass treatment can be suspended.
India
In India, we partnered with national research institutions to assess impact across 11 states. Three states now have published data showing dramatic declines: Himachal Pradesh and Rajasthan both reduced worm prevalence to below 1%, while Chhattisgarh cut prevalence from 75% to 14%. These results position states to scale down treatment in line with WHO guidelines.
Where funding gaps threaten progress
In Pakistan, we support deworming for over 14 million children annually, and are now supporting impact assessments to measure changes in prevalence and inform future treatment strategy. We estimate that 3-5 more treatment rounds could help Pakistan reduce prevalence down further to enable reductions in the scale of the program and hand over the program to the government. But the program is facing funding limitations and may wind down prematurely without additional support. Pakistan is often overlooked by global health funders: despite having a similar population and health indicators to Nigeria, it receives just one-third of the development assistance. This disparity makes philanthropic investment all the more critical.
In Malawi, more than 50% of children suffer from parasitic worm infections and anemia. In 2024, we launched an integrated school-based health program that combines deworming with iron and folic acid supplementation — an innovative model that reduces costs by 12% while addressing both conditions through a single delivery platform. By year three, we'll reach 3.5 million children for less than $1.35 per child per year. We've secured funding for the program through 2027, but we anticipate a few more years of technical assistance will be needed to curb parasitic worm infections and build lasting government capacity. We're seeking partners to fund the program through 2030.
In Tanzania, we've launched a new partnership to prevent disease resurgence amid national funding shortfalls. Thanks to support from Founders Pledge, this work is moving forward — proof that when funders step in at the right moment, progress continues.
The math is clear
Deworming remains one of the most cost-effective health interventions available — as little as 7 or 8 cents per child in some of our programs. Every $1 invested generates approximately $169 in economic returns to children's livelihoods.
The infrastructure is in place. The governments are committed. The communities are ready and waiting. What remains is the funding to see it through.
We call on philanthropic partners to fill the gaps left by declining aid. Evidence Action has proven we can deliver results at scale. With your support, we can finish the job — before this window closes.
Deworm the World in photos

Nsanje, Malawi
Nsanje, Malawi: Rose Patrick, an 11-year-old at Makoka primary school, accepts a deworming tablet during a school-based treatment event.

Haryana, India
Haryana, India: Garvita, a student in Haryana, India, holds up a sign she created about the effects of parasitic worm infections during a National Deworming Day event in February 2025.

Ogun, Nigeria
Ogun, Nigeria: Students gather outside of Ositelu Memorial College ahead of the Nigerian school's first deworming event.

Chikwawa, Malawi
Chikwawa, Malawi: Primary school children celebrate after a school deworming event in November 2025.
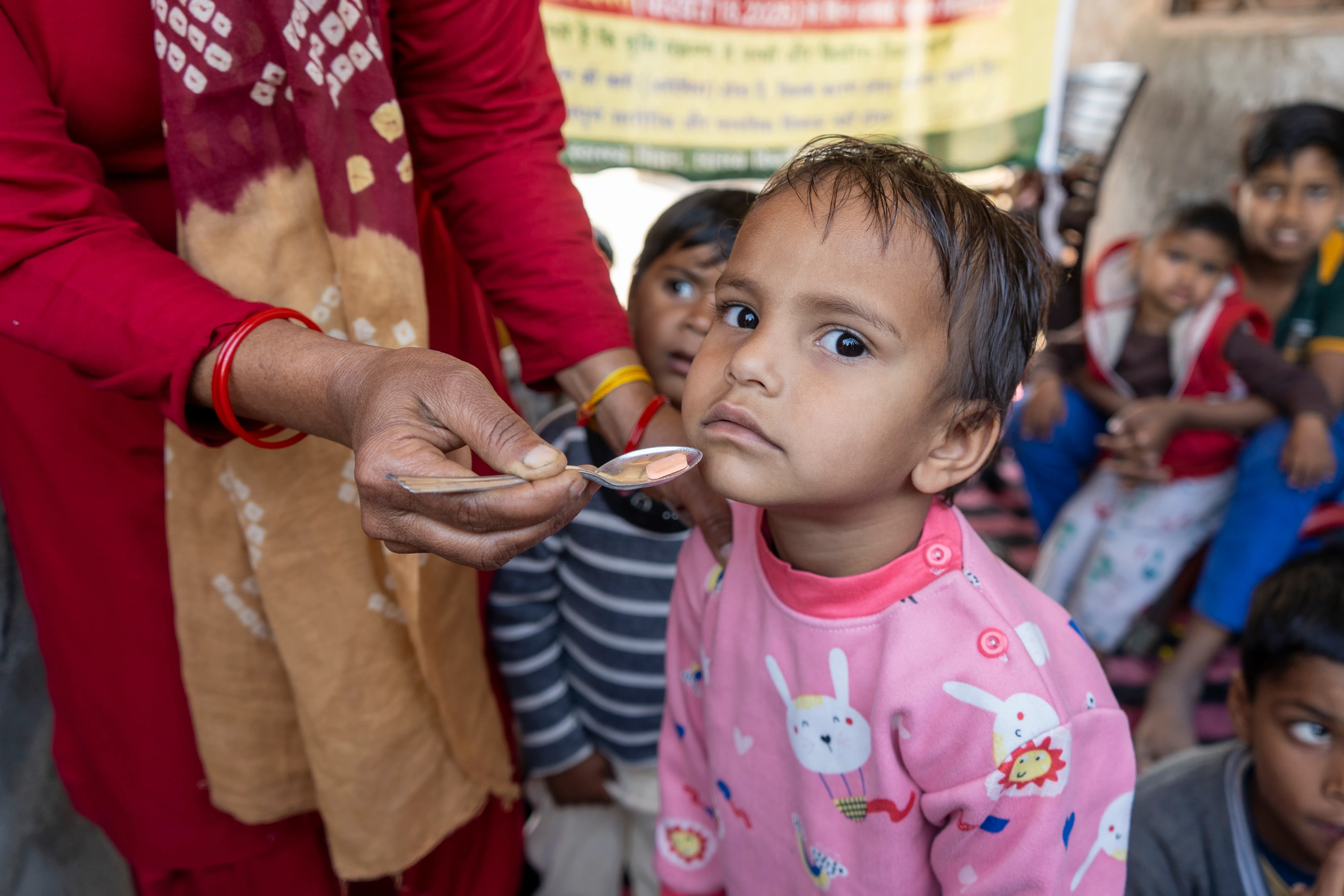
Haryana, India
Haryana, India: A child prepares to accept a deworming tablet during the National Deworming Day event in February 2025.
Where we're making progress
From India's massive National Deworming Day to new partnerships in Tanzania, Evidence Action is helping governments deliver treatments at unprecedented scale.
Pakistan
In October 2025, we launched the National Impact Survey for Pakistan’s deworming program, which we’ve supported since 2019 and now reaches about 14 million children annually. Using microscopic analysis of stool samples to measure prevalence and intensity of worms, the survey will measure the impact of the deworming rounds to inform program strategy going forwards.
At the same time, we’ve continued to work with the provincial governments to mobilize domestic resources towards the program, strengthening its long-term sustainability. As a result of these efforts, the government of Khyber Pakhtunkhwa recently made a three-year allocation to support 20% of the annual implementation budget. This represents a significant milestone and sets an important precedent for other provinces to follow.
India
After a decade of sustained treatment supported by Evidence Action, several Indian states have eliminated parasitic worms as a public health problem. In 2025, we scaled back or concluded our support in these states as they demonstrated the capacity to maintain programs independently.
In August 2025, National Deworming Day — one of the world's largest single-day public health campaigns — delivered treatment to 146.8 million children across the three states where we continue to provide full technical support, maintaining the massive scale we've achieved over the past decade.
We anticipate all Indian state programs will operate independently by March 2027, proving that technical assistance can be time-bound and that government systems can fully own proven interventions.
Nigeria
After seven years of partnership in Cross River State, our technical assistance helped reduce prevalence of soil-transmitted helminths by 49% and schistosomiasis (a waterborne parasitic disease) by 75%.
The recent results – collected in partnership with the Cross River state government – informed the state’s decision to reduce treatment frequency in areas where worm prevalence is now low. This approach ensures that resources are allocated more effectively and targeted to communities with the greatest need.
Kenya
Since we began supporting Kenya's national deworming program in 2012, worm infections have dropped over 80%, meaning millions of children now avoid the anemia, malnutrition, and school absenteeism these infections cause.
This progress positions Kenya to eliminate worms as a public health problem by 2027. Thanks to strong government capacity and commitment, we're now exploring our pathway to conclude our technical assistance and provide the government with the tools and resources they need to keep worm infections under control.
Tanzania
In 2025, we expanded our footprint to Tanzania to help build a smarter, more targeted system for reaching the more than 10 million children still at risk of parasitic worm infections.
Rather than immediately launching mass treatment campaigns, we're starting our partnership with what Tanzania needs most: evidence. In 2026, we’ll conduct the first nationwide prevalence survey in over 20 years, enabling the government to shift from country-wide treatment to focused delivery in high-burden areas. This support will enable the government to potentially halve the number of districts requiring treatment while ensuring children who need care most receive it.
Malawi
We successfully scaled the program to 15 districts, expanding our reach to more than 1.3 million adolescent girls with weekly iron folic acid supplementation. By layering iron and folic acid supplementation with the deworming program, we deliver both interventions through schools using the same trained health workers and teachers — reaching children where they are while keeping costs low.
With 50% of Malawi's children currently infested with worms, anemic, or both, we have a clear path to national coverage in 2026, demonstrating how this layered approach can address multiple health challenges simultaneously at scale.